CDC Reports
Increasing Incidence of Liver Cancer, Mostly Due to Chronic Hepatitis
B and C
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
The
number of new cases of hepatocellular carcinoma (HCC),
a type of primary liver cancer, has increased in the
U.S. over the past several years, reaching an incidence
rate of 3.2 cases per 100,000 persons in 2006, according
to the latest figures reported by the Centers for Disease
Control and Prevention (CDC) in the May
7, 2010 issue of Morbidity and Mortality Weekly Report.
Blacks and people in the 50-59 year age group had the
largest annual percentage increases in HCC. |
|
 |
 |
 |
 |
 |
 |
 |
By
Liz Highleyman
Over
years or decades, chronic hepatitis
B virus (HBV) or hepatitis C
virus (HCV) infection can lead to serious liver disease including
cirrhosis and HCC.
Liver cancer is the third leading cause of cancer death worldwide
and the ninth leading cause in the U.S.
More
than three-quarters of all liver cancer cases are thought to be
attributable to hepatitis B or C; other causes include heavy alcohol
consumption and genetic diseases of the liver. While the incidence
of new HBV and HCV infections has declined dramatically, liver
cancer rates continue to increase as people infected long ago
reach the stage of developing advanced liver disease.
To
determine trends in U.S. HCC incidence, CDC researchers analyzed
data for 2001-2006 (the most recent available) from CDC's National
Program of Cancer Registries and the National Cancer Institute's
Surveillance, Epidemiology, and End Results (SEER) system. They
compiled reports from 45 cancer registries, covering 90.4% of
the U.S. population. Only microscopically confirmed HCC cases
were included in the analysis.
Results
 |
A
total of 48,596 new HCC cases were reported during 20011-2006. |
 |
The
average annual HCC incidence rate during 2001-2006 was 3.0
per 100,000 persons. |
 |
The
incidence rate increased significantly over the study period,
from 2.7 per 100,000 persons in 2001 to 3.2 per 100,000 persons
in 2006. |
 |
The
average annual percentage change (APC) in the HCC incidence
rate was 3.5%. |
 |
Men had about 3 times higher risk of developing HCC than women
(5.0 vs 1.3 per 100,000 persons), a disparity recently
linked to androgen receptors. |
 |
HCC
annual incidence rates increased for both men (from 4.5 to
5.4 per 100,000) and women (from 1.2 to 1.4 per 100,000) between
2001 and 2006. |

|
The
median age at HCC diagnosis was 64 years (62 for men, 69 for
women). |

|
The
highest HCC incidence rates were seen among people in the
70-79 year age group (13.7 per 100,000 persons), followed
by age 80 or older (10.0 per 100,000), 60-69 years (9.6 per
100,000), and 50-59 years (6.8 per 100,000), then dropping
in the 40-49 year group (2.1 per 100,000). |

|
The
greatest increase in incidence, however, was in the 50-59
year age group (APC 9.1). |

|
Asian/Pacific
Islanders had the highest HCC incidence rate (7.8 per 100,000
persons) -- reflecting their high hepatitis B prevalence --
followed by Hispanics (5.7 per 100,000), blacks (4.2 per 100,000),
American Indian/Alaska Natives (3.2 per 100,000), and whites
(2.6 per 100,000). |

|
The
largest increases in HCC incidence were seen among blacks
(APC 4.8) and whites (APC 3.8), while it remaining stable
among Asians. |

|
HCC
incidence rates varied widely among states, ranging from 1.4
per 100,000 persons in South Dakota to 5.5 per 100,000 in
Hawaii. |

|
States
with particularly large annual increases in HCC incidence
included Oklahoma (+11.7%), Maine (+9.9%), Iowa (+9.0%), and
Georgia (+7.4%). |
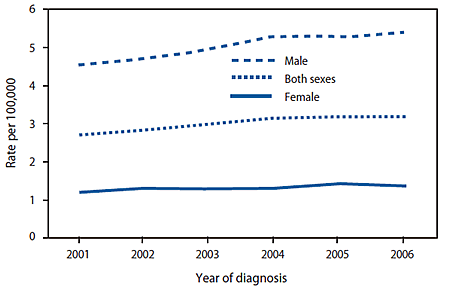
Graphic
caption: Hepatocellular carcinoma incidence rate by sex --
United States, 2001--2006 (Source: CDC).
"The
results demonstrate a continuation of long-term increases in HCC
incidence and persistent HCC racial/ethnic disparities,"
the researchers concluded.
"Development
of viral hepatitis services, including screening with care referral
for persons chronically infected with HBV or HCV, full implementation
of vaccine-based strategies to eliminate hepatitis B, and improved
public health surveillance are needed to help reverse the trend
in HCC," they recommended.
In
an editorial note, the authors explained that HCC rates were highest
among people born during 1946-1964, particularly so among black
men. "In the absence of testing and care," they wrote,
"the risk for HCC is expected to increase with aging of the
cohort of persons with HCV infection."
Timely
treatment for hepatitis B or C reduces the risk of developing
liver cancer. People with chronic liver disease should be screened
for HCC, since the chances of successful treatment are better
when the cancer is detected at an earlier stage.
"Early
identification of viral hepatitis with referral to prevention
and care services can decrease transmission to others," the
authors stated. "Treatment of viral hepatitis is cost-effective,
and medical management can decrease morbidity."
A
recent report on prevention of hepatitis and liver cancer from
the Institute of Medicine called for a national comprehensive
approach comprising improved viral hepatitis surveillance, community
education, vaccination to eliminate HBV transmission, and development
of prevention and health services targeting key populations (i.e.,
drug users, foreign-born individuals, and HIV positive people),
including HBV and HCV screening and linkage to appropriate medical
care.
Investigator
affiliations: Division of Viral Hepatitis, National Center for
HIV/AIDS, Viral Hepatitis, STD, and TB Prevention; Division of
Cancer Prevention and Control, National Center for Chronic Disease
Prevention and Health Promotion, CDC.
6/15/10
Reference
S O'Connor, JW Ward, M Watson, and others. Hepatocellular carcinoma
-- United States, 2001-2006. Morbidity and Mortality Weekly Report
(MMWR). 59(17): 517-520 (Free
full text). May 7, 2010.
