Numerous
studies have found that HIV
positive people are at higher risk of cardiovascular disease
than their HIV negative counterparts, which may be attributable
to persistent infection and resulting inflammation, antiretroviral
therapy (ART), or some combination of these and other
factors.
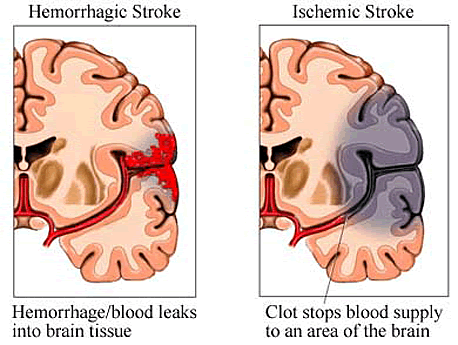
Caused by interruption of the brain's blood supply, strokes
are classified as ischemic, due to blockage of blood flow
(for example by a blood clot), or hemorrhagic, due to bleeding
in the brain. The ischemic type can be an outcome of atherosclerosis,
or buildup of cholesterol, cell debris, and other material
in arteries.
Strokes
are often included among the cardiovascular "events"
recorded in such studies, but they have not been the focus
of much separate research. However, they are an increasing
concern as the HIV positive population ages.
In the present analysis, Bruce Ovbiagele from the University
of California at San Diego and Avindra Nath from Johns Hopkins
University looked at trends in the proportion and number of
HIV positive individuals among stroke patients in the U.S.
The investigators collected data from all states that contributed
to the Nationwide Inpatient Sample, and identified all patients
admitted to hospitals between 1997 and 2006 with a primary
diagnosis of stroke.
Results
 |
Looking
at both ischemic and hemorrhagic strokes combined, HIV
positive people made up 0.09% of all patients hospitalized
with strokes in 1997, rising to 0.15% in 2006, a significant
increase. |
 |
Looking
at only ischemic strokes, HIV positive people accounted
for 0.08% of hospitalizations in 1997, rising to 0.18%
in 2006, again a significant jump. |
 |
The
proportion of HIV positive people among patients with
hemorrhagic strokes, however, did not change significantly
during this period. |
 |
In
terms of actual numbers, 888 HIV positive people were
hospitalized with strokes in 1997, rising to 1425 in 2006,
a 60% increase that was largely attributable to more people
living with HIV. |
 |
During
the same period, in contrast, the overall number of stroke
hospitalizations among the general U.S. population fell
from 998,739 to 926,997, a 7% decrease. |
 |
The
rate of strokes began to increase notably in 2001, increasing
from 90 to 129 stroke hospitalizations per 100,000 HIV
positive people between 2001 and 2006, a rise of about
43%. |
 |
The
median age of HIV positive people at the time of stroke
hospitalization rose from 43 years in 1997 to 48 years
in 2006. |
 |
In
a multivariate analysis, stroke patients receiving Medicaid,
those in urban hospitals, and those with dementia, liver
disease, kidney disease, or cancer were more likely to
be HIV positive. |
"Over
the last decade in the United States, there has been a substantial
and significant rise in patients hospitalized for stroke with
coexisting HIV infection," the study authors concluded.
"This has important public health and socioeconomic consequences."
"The median age for stroke in this [HIV positive] population
was the fifth decade, which is much lower than that of the
non-HIV-infected population," they elaborated in their
discussion. "This indicates that HIV infection or its
treatment is directly related to the stroke pathophysiology
in this population."
HIV
infection could potentially cause strokes via several mechanisms,
they continued, including endothelial activation leading to
accelerated atherosclerosis, opportunistic infections, cancer,
and HIV-related heart disease, blood vessel dysfunction, and
metabolic abnormalities. But it is unlikely that HIV is more
apt to cause such problems now than it was in 1996.
A
more plausible explanation, they concluded, is that the advent
of effective combination ART in the mid-1990s allowed more
people with HIV to reach an age at which the risk for strokes
starts to increase.
Beyond
that, "longer exposure to HIV, even at low viral load
levels, may allow for the direct effects of the virus to increase
stroke risk," they suggested. In addition, prolonged
use of antiretroviral drugs may contribute to metabolic, blood
vessel, liver, and kidney problems that can play a role in
ischemic strokes.
Fortunately,
strokes are "highly preventable," Ovbiagele told
HealthDay, with lifestyle changes such as weight loss, controlling
cholesterol, and quitting smoking.
Investigator affiliations: Stroke Center and Department
of Neuroscience, University of California at San Diego, San
Diego, CA; Division of Neuroimmunology and Neurological Infections,
Department of Neurology, Johns Hopkins University, Baltimore,
MD.
1/28/11
Reference
B Ovbiagele and A Nath. Increasing incidence of ischemic stroke
in patients with HIV infection. Neurology (Abstract).
January 19, 2011 (Epub ahead of print).
Other Source
R Dottinga. Stroke Risk May Be Higher in HIV Patients. HealthDay.
January 19, 2011.
